
My loving wife Cheryl
Age: 61
Location: MI
Became sick: 12/25/2021
First sought care: 12/27/2021
Admitted: 01/05/2022
To: South Bay hospital
Murdered: 01/16/2022
Cheryl Corsi




The purpose of this letter is to document the frustrating and fatal medical decisions made without my permission as medical power of attorney, that ultimately led to the death of my husband Dennis Burgess in February of 2022. He was a healthy physically active retired businessman, a Vietnam veteran, and avid sports mans. He was a generous contributor of time and talent. He was a great resource to his community. He had always been physically active. We live on an acreage with riding horses. We went camping and boating in the summer. We wintered in Arizona for 3 months at a time. During our time in Arizona, we rode our razor with friends and he played golf with friends. Denny played 18 holes of golf two days before he became ill with covid. We had elected not to have the covid vaccine when it was first available because we were certain we had had covid when the public was first informed of its presence here in the United States 2020. Following that we had been exposed to by relatives and friends who had tested positive for covid infection and we never came down with it. Our daughter who works in the medical field told us about patients who were developing myocarditis, blood clots in their lungs, strokes, and stomach problems. We thoroughly researched the side effects and felt that the vaccine had not been sufficiently tested.
Here is the scenario that led to our tragic loss, which began with a simple bout of pneumonia. Denny became ill in September of 2021 with pneumonia. He was misdiagnosed the first time going to the urgent care in which they misdiagnosis him with strep throat. He went back to the doctor after finishing the first round of antibiotics and we requested he get a chest x ray which at that time they diagnosed him with pneumonia and started a stronger antibiotic. He suffered two bouts of this. Denny was tested two different times for covid and both times he tested negative.
In November 2021 I started having symptoms of covid and took a at home test right away it came back positive so I went to the urgent care where I was asked if I wanted an infusion of monoclonal antibodies which I did and they ordered them for me. Denny became ill 2 days later. He tested positive for covid with an at home test so he went to the urgent care and was asked if he wanted the monoclonal antibodies which he did want the infusion. He also had another chest x ray at that time that showed the pneumonia had come back. He was given another prescription of antibiotics that he had previously been on but the order for the infusion was not acted on by his PPO Carrie Benn for three working days. It was 5 days after the positive test that the order was passed on. He was given the infusion of monoclonal antibodies at Mercy Medical Hospital 11.15.2021.
There is no medical record from Mercy Hospital saying it was ordered or given. Meanwhile Denny just kept getting worse. I took him to Unity Point Hospital St. Luke’s in Cedar Rapids Iowa on November 19th 2021. This was 10 days after the initial symptoms. The hospital would not let me or our daughter go into the ER with him. We sat in our car for 6:00 am till 3:00pm to learn what treatment they anticipated doing. We Specifically told them not to intubate him or use a ventilator or use Remdesivir. The nurse in charge told us we had no right to dictate his care even if I had medical power of attorney. At first the nurse stated that Denny was confused, but when we informed her of our medical power of Attorney status, she insisted he was of sound mind and could make his own medical decisions. We told her we planned on contacting our attorney. She replied she was going to have us investigated for elderly abuse because he was so ill.
The following day a social worker called me and interrogated me. I am a retired nurse with years of experience. Subsequently we did not see him for 3 weeks and only talked to him by phone 2 to 3 times. On his cell phone. When we called and asked to speak to him the staff told us his phone needed to be charged. He had his charging cord with him. They said they would charge the phone when they had time. We brought Denny food, but had to leave it at the hospital entrance. The staff treated him with procedures of which we were not aware of. They tried to intubate him which in medical records said it was pulled out. They wanted to catheterize him and he told them no they would have to call us. When they called we said no it would just introduce more pathogens in his body. He was not incontinent. They went ahead and did it anyway.
He fell in the shower or bathroom. One doctor denied it happened, another said it did. He was given Atavan numerous times despite the fact that he was allergic to the drug and had to be strapped down in the bed after he blacked out from receiving atavan. My Daughter and I told the staff No Atavan and this information was supposed to be put in his chart. They administered 120mg of steroids in IV Solumedrol. This is a large dose normal dose is not to exceed 40 mg orally according to our family doctor. On Thanksgiving day he was given 3 medications which threw him into a state of shock with a blood pressure reading of 70 over 49. He was transferred to the ICU for 24 hours. The staff claimed they did not know what caused the Blood pressure to drop. A caregiver came in and told Denny they thought he had an allergic reaction to medication that he was given. He asked for towels and soap and water so he could clean himself up after bowel movement. After waiting 4 hours or more they gave him 2 baby wipes to clean himself up. He was too weak to get up. He had one shower in 3 weeks after being at the hospital. Twice he was given large baby wipes for bed baths. He received very poor care from Dr. Azam and his staff on the pulmonary care floor. The nursing supervisor was MaryBeth Keuther of pulmonary floor. When we called with our concerns of care for Denny she said That this is why they call “ it practicing nursing not nursing perfection”. She said “ there is no perfect nursing care”.
When he was taken for a cat scan of his lungs. He had a nasal cannula mask for his breathing but then he had a plastic bag over his head. He said it felt so demeaning and claustrophobic to him.
He was transferred to physical therapy for a week and received better care on this floor. We were finally able to come see him. Here they started having him doing exercises. They got him up to shower which he felt so much better with showering. He got to get up and sit in his chair in his room. He was doing very well with therapy. He was going home with oxygen at 4 liters. One of the days I was there visiting him, the nurse taking care of him came in and said “ he was one of the lucky ones” He was sent home on December 16th 2021. He was improving each day he was walking one mile in the house, doing leg lifts and squats. He was exercising his arms.
He had an appointment with the lung doctor on 1.04.2022. But when we arrived the doctor was not even there we had to see a Nurse practitioner who was very negative. She told him he would probably never be able to get off the oxygen and would be in a wheelchair the rest of his life. He saw another nurse practitioner the next Thursday 1.6.2022 which was a pointless trip into negative 25 degree weather just to ask him how his exercising was going at home. Two receptionists in the waiting room were sick and coughing. We were decreasing the steroids down to 20 mg a day. Denny started having panic attacks and having to turn his oxygen up to catch his breath. His Blood level of O2 would drop during the panic attacks and then when we could calm him down then it would come back up.
One night two days after we had lowered the steroids from 20 to 10 mg. Following the doctor’s orders to taper every 5 days. Denny had a very bad panic attack and we couldn’t get the at home oxygen machine to go high enough to help him catch his breath. We had to call an ambulance to take him to the hospital. His O2 was only 42 when the ambulance got to our house. They immediately put him on Bi pap on the way to the hospital. The ER doctor said that they see this often when tapering off steroids. They were going to keep him for observation overnight in the ICU and probably let him go home tomorrow. He ended up being in the ICU for 3 days. There he was started back up on high doses of steroids but not given his blood pressure medication. The Oxygen face mask did not fit him properly. The nurse accused him of removing it. We asked for water for him to drink, his mouth and lips were so dry. When he was drinking his water he coughed and the nurse told him that he was drinking his water too fast and that he was going to aspirate if he didn’t slow down. She then told him he would have more tubes coming out of himself in places he wouldn’t like. My daughter and I were sitting there listening to the whole thing. We said “he has a slight cough and he is not aspirating his water”. She said she would intubate him if she needed to and then She just smiled and shrugged her shoulders and walked out of the room. Denny was scared to death after she said that. The second day when he was there he was eating and the same nurse said if you don’t slow down while eating your food you are going to aspirate and then I will be intubating you, we were both there again and told her that will not be happening we won’t let it. Again she just smiled and left the room. At this point he was not sleeping well at night.
He was moved to the 6th flood pulmonary unit where he was before on his prior stay in the hospital. They put him on a 500 calorie diet. There was no water pitcher or glass of water at his bedside. And he was not able to use his spirometer. No respiratory therapy was done. We asked for flutter valve and compression vest treatment. The staff did it once, then removed it from the room. He was having panic attacks. His medication included 120mg of steroids, atavan which he was allergic to, trazodone, morphine which through this whole thing he had NO PAIN. Percocet and another tranquilizer for schizophrenia, plus sedation medicine. He was never given IV fluids. He became dehydrated. There were two lung specialists in the hallway arguing about the dosage of steroids being given. One said the doses being given were too high and the other said it was fine. Denny was getting weaker and very depressed everyday. We had requested a transfer to the UIHC because they gave him atavan and he blacked out for 24 hours. He couldn’t remember anything that happened the night before. They told us that they could not transfer him because the other hospital would not accept transfers right now. They then went in and talked to Denny telling him that they were doing the best they could and that the other hospital couldn’t do anything different that they weren’t already doing. For the next 3 days when the doctor would come to see him he told him he was not going to get any better and that if he would have gotten the covid vaccine he would never have been in this situation in the first place. He told Denny that they didn’t have a single person in the hospital with covid that was vaccinated; it was all the unvaccinated. That same doctor started to taper him again off the steroids. Thursday that week the doctor requested a palliative care team come talk to Denny without the family knowing. Denny called our daughter to come talk to him as soon as possible so she did and he said they wanted to give him a percocet to help him with bowel movements. Two Saturdays after he went into the hospital, Our daughter went to see him and the nurses had left him in his chair after breakfast asleep and his O2 was in the 80’s.He told our daughter he had been asking to go back to bed but they just left him in the chair upright sleeping. Our daughter requested he go to bed while he slept so the nurse came and got him into bed. The nurse practitioner told our daughter that his lungs sounded good and that they might fit him for a bi pap mask and he might get to come home the next week. But then an hour later another doctor came in and said that they were going to up his steroids and start him back on a bi-pap mask because his O2 were in the 80’s,so they needed to get him back up into the 90’s . The nurse kept turning the oxygen up and down before they put him on the bi pap machine. Denny was then very scared and was also experiencing claustrophobic feelings with the mask on. The mask didn’t fit right and Denny was having a hard time with keeping it on. The doctor came back in and said if he couldn’t wear the bi pap mask she was going to have to put him on a ventilator. Our Daughter said no we refuse him being put on a ventilator. The doctor said she was going to give him atavan to relax him to keep the bi-pap mask on. Our daughter said no it should be in his chart he can’t have atavan he blacks out. This information was supposed to be in his chart. Our daughter had written it on the board in his room and we had told the staff countless times no atavan. So the doctor said she would give him trazadone which he had done fine with. What we didn’t know was they also gave him percoset 325mg which has 25mg of oxytocine. The percoset was ordered by the palliative care team, as well as the morphine and other mind altering drugs. The room was darkened and soft music was played. We as a family nor did Denny request palliative care get involved. The team began to discuss the end of life with him. I was not notified of any of this even with a medical power of attorney. He was given insulin and lasix even though he was not experiencing heart failure nor was he a diabetic. When I questioned the nurse about why they would be giving it to him she said that it was ordered by the doctors. I said but he is not a diabetic and he is not in heart failure. We asked to speak to a doctor. They said they were very busy and could not discuss his care with us till Wednesday.
Denny was not given a bath for 2 weeks he developed bed sores. Physical therapy and respiratory therapy was discontinued. He was so over medicated he could not even hold his head up. His weight was 181lbs when he went into the hospital which was a healthy weight for him. He ended up weighing 159lbs in two weeks. We had requested a family meeting with the care team on Friday morning but they would not meet with us till Wednesday January 26th the next week. The Monday before the meeting all he was doing was sleeping we couldn’t barley get him to even open up his eyes we kept asking the care team why such a change they all kept telling us that we would have to wait till Wednesday meeting to find out they could not discuss his care with us till then. Tuesday morning before the meeting my daughter and I went up at 6am at the start of visiting hours like we had been doing every morning. We woke up Denny from sleeping to talk to him. My daughter told him we were very worried about him. We told him he had been sleeping so much that he had not gotten out of bed since Sunday morning. We told him he was beginning to get puffy and we were so worried about him. He was very confused when we told him this. As our daughter was trying to talk to him. The head floor nurse MaryBeth Keuter came rushing into his room and started talking very loudly. She told us we were using very hurtful words with Denny and she was going to have to ask us to leave. My daughter said “wait a minute what is so hurtful about trying to help get her dad to realize that he is getting worse not better”. She said we need you two to leave for a while the nurses come get his vitals and weight him. We agreed to wait outside the room but we were not leaving. She said if they hear us discuss anymore of his medical care with him we will not be able to come back to see him. Our daughter asked to sit down and talk with with her. She agreed. We talked with her for about 30 minutes explaining we just want the best for him, we want him to get better. She just kept telling us that we would find out more in the family meeting. She wanted to know why we thought we knew so much about the medical field. We explained that I was a retired nurse and our daughter is a sonographer. She just kept smiling and telling us we would find out at the family meeting and that until then we were not to discuss his medical care with him. We agreed so that we could continue to see him. Our daughter left and went to work while I went back to the room to sit with Denny. Later in the morning Dr. James Bell from the palliative care team stopped in to see Denny and asked me to step out of the room so he could talk to Denny alone. He then came out of the Denny’s room and told me that Denny didn’t want me there and that I needed to leave. 01.25.2022 The Percocet and morphine were increased to every 4 hours whether he needed or not. I was advised by my attorney to have a statement notarized stating as Denny’s medical power of attorney I did not want him to be given anymore or increased sedation medication that would knock him out. 01.25.2022. Tuesday night our daughter received a phone call asking why no one came to see him that night. We said well your Dr. requested that we not come till tomorrow for the family meeting. He then called Me and asked why I hadn’t come down to see him. I said Dr. Bell told me you said you wanted me to leave and not to come back till the next morning family meeting. Denny said stop playing games with me. I said I’m not. I was told that if we didn’t listen to them we wouldn’t get to come see you at all. Denny said I’m just so confused on what’s going on here with my medical care. I said we are trying to help you but they won’t let us. He told me that he never said that he wanted me to leave today. That Dr. Bell lied. We talked and he said he would just see us in the morning.
The morning of the Palliative care/ Family meeting we were only allowed to have two family members in the room, while they had an ARNP Emily Fye from palliative care, a chaplain and we requested a care coordinator. Our other children and Denny’s brother were on the phone listening. During this meeting Denny was so sedated again he couldn’t keep his eyes open. He slept during the entire meeting. The questions such as Denny do you want to start end of life processes ? Then they would say Denny do you agree? He said yes with his eyes closed. The ARNP Emily Fye asked him if she could take off his full code wrist band and replace it with DNR. He did not answer so she had to say Denny and he said yes. So she cut it off and put the DNR on as quickly as she could. I said we don’t give consent to this and I’m his medical power of attorney. The ANRP Emily Fye said you don’t have authority because he is of sound mind. My daughter and I said really he can’t even keep his eyes open and you are spoon feeding him and taking his yes answer good enough. He is not of sound mind, he is so drugged up he doesn’t have any idea what is going on right now. Denny was replying yes to his name not to the questions she was asking him. She said he is not going to get any better and this is what he wants. You can’t stop it. The minister told a story about how Dad and him had walked up the mountain and asked God to sacrifice a lamb instead of taking Denny and God didn’t so it was Denny’s time to end his life. We felt like we were in the biggest nightmare of our lives. We said we were requesting for the second time to be transferred to the UIHC. They said there was nothing more that UIHC would do for Denny that St. Luke wasn’t already doing for him. It would be a lateral transfer which was not true. Then Emily Fye said they wanted to get this started as soon as possible, Denny’s brother asked if they could wait till he could get back home from Arizona to say goodbye to him she said I suppose but he needed to hurry so that they could get it started soon. We asked if we could take him home and she said we have a very nice hospice unit right down the hallway he could be moved to but she would not let him leave the hospital because she didn’t think Denny would make it to our house or the University of Iowa hospital and clinic without dying in the ambulance. Emily Fye told us that it would take two days for Denny to pass. She asked Denny if he wanted to move rooms but she didn’t think he should. We said just leave him in this room. She said she was done for now and that she would start the orders for Monday the 31st to start the end of life so that Denny’s brother could come see him one last time. Then she left the room. We were in shock. My daughter went out to the nurse desk which it was right across the hall of his room and when she entered the hall all the nurses including the nursing supervisor were huddled around the Patient TV monitor watching our meeting as if it was a TV show they had been watching. My daughter Startled them when she walked up. There must be a delay in the TV from the room. They all started working as if they hadn’t been watching us. My daughter asked if we could take him off of his 500 calorie diet now that they had him on end of life protocol so we could start to bring him some of his favorite food. The nurse said oh yes that’s fine without even talking to a doctor. But before when we asked about it they said nope we have to follow doctors orders. We asked the doctors about it and they said it was a heart healthy diet.
My daughter and I left for a while to discuss the news we had just been given with our family. We refused to believe this is what Denny really wanted. My other daughter and I went back to the hospital taking Denny, his favorite Mexican food. He was more alert at this time the sedation medication that they had given him that morning was wearing off . He ate a good meal and his spirits were coming back just a little. He had enough strength after eating to get up and walk to the other side of the room. He did leg lifts. It was unbelievable. Really this whole thing is unbelievable still is. We had a heart to heart with him. We begged him to sign himself out because they wouldn’t let us use our medical power of attorney. Denny agreed and we called an area ambulance to come pick him up at 8pm and drive him to University of Iowa hospital and clinics. Denny required oxygen otherwise we would have just taken him ourselves. Denny was required to state verbally and sign documents stating he was leaving against medical advice on his own free will. The lung specialist on duty Dr. Azum would not release him. He stood in the doorway trying to block it. Telling us we couldn’t do this. My daughter said we just did and you can’t stop us now get out of our way now. The head nurse threw a tantrum and threw the papers at us to have Denny sign.
When we arrived at the emergency Department at the UIHC they could not believe the medications (over sedation) and lack of care Denny had been receiving by St. Luke’s hospital. UIHC had to give him two baths in the middle of the night when he was admitted to the unit because he was so dirty. They started wound care on his lower back where he had a bed sore. They did CT and a whole bunch of test that night.
Our daughter went to be with him that next morning because he could only have one visitor per day at the University of Iowa. The care team came in that morning and said that Denny at this point they felt he needed a lung transplant. That if he agreed and we agreed then they would start the process right way of getting him on the list. We agreed that if that’s what it took we would do anything to get him well. St. Luke’s hospital had Denny on so many mind altering drugs and high doses that the UIHC said they had to get him off of them to be able to get him on the transplant list. So they took him from 120 mg of steroids down to 40 mg. He was being tapered from 40mg down because he could only be on 10 mg in order to be eligible for the lung transplant. They took him off of the percoset and morphine immediately . He was going through drug withdrawals. He said he felt like his skin was crawling off of his body. He felt like he was on fire at one point. Our daughter was rubbing him down with a cold wash cloth. Trying to help him. He said he was seeing things and he was so scared his panic attacks were getting worse everyday that he was there. He called my mom in the middle of the night the second night crying saying he was so scared.
They ran multiple tests including cardiac cath and tissue sampling which they had to have signed consent from his medical power of attorney before they would do the tests. All the tests came back and he had the body of a 50 year old man. They said he was not in congestive heart failure like St. Luke’s had said he was not a diabetic and that he was elegible for the lung transplant list. They said to bring him any healthy food he would eat because he had lost too much weight but they didn’t really order him food unless we did it for him.
On 02.01.2022 when I got there to see Denny the curtains were drawn, the lights lowered and lower music played by the nursing staff. One respiratory therapist told him he would not be in this situation if he would of received the covid vaccine.
The day before Denny’s death the lungs specialist said everything is a go for the transplant list. 02.03.2022 and that his name would be put on the top of the list because his lungs are in such bad shape. There was a lady that came in with the transplant team that was yelling at Denny asking him if he could stand pain? He kept saying yes I can stand pain. She asked him if he had ever been in severe pain? He said well when I had kidney stones and broken ribs once. She asked him if he was in pain now? He said he has had no pain this entire time, just panic attacks. Which made him feel like he couldn’t breath. The other two doctor’s said they would be able to help him manage his pain and not to worry about it. The other woman kept telling him abusively about how they were going to cut him from one end of his chest to the other end and crack open his ribs. She said you think you can withstand that kind of pain? Denny’s eyes got real big. He said I will certainly try. Then all at once they said they had to go see another patient. Denny said he had a couple of more questions for them could they come back. The lady said she would stop back by later. I waited till 6:00 pm an hour after visiting hours ended at which I was asked to leave. I think that lady came back in after I left and talked him into ending his life.
The following morning Denny’s brother came to visit and before he got to the hospital, Denny had taken himself off the transplant list and started end of life. He told his brother that something came to him in the middle of the night and told him it was time to go home with god. Denny was depressed from all the steroids, opoids, and tranquilizers and sedation medication he was on and then taken off so quickly. He was having hallucinations since the first hospitalization. He was suffering from steroid psychosis and in a steroid crisis. Unknown to us the end of life team had been coming to see him without our requisitioning this and without our permission even though I had medical power of attorney. He was not of sound mind to make the decision to end his life. There was no verbal or written request written from Denny or his family to proceed with this procedure. Ironically when he had his cardiac catheter 2 days prior I had to sign a written permission for that. So why not for the end of life? When his brother arrived to see him at the beginning of visitor hours at 9am , Denny had already received his first high dose of morphine to start the process of ending his life. We as his family were not notified that this was happening. He could of died without me or our children knowing what was happening and having a chance to be by his side had his brother not contacted us.
I feel St. Luke’s hospital should be investigated for poor medical and nursing care, elderly abuse and for failing to inform the family of medication he was being given. Also for treatments which they were not authorized to do, stopping IV fluid there by dehydrating him and stopping his antibiotics . They verbally abused him everyday telling him it was his fault he was in this situation and if he would have been vaccinated for covid 19 he would never have been in the hospital. They told him everyday he was not going to get better, he would be hooked up to the oxygen tank for the rest of his life. They then told him if he didn’t want to live like that they could help him with end of life. He was confused and drugged while they were doing this to him. The University of Iowa end of life team simply completed the unfortunate series of events. The action of the palliative care/ end of life team was not compatible with the normally high standard of care that the university of Iowa hospital delivers. I am hoping that the failures in Denny’s care will be investigated so that no other family has to suffer the grief we have suffered. Denny’s death was preventable. We have contacted 2 lawyers and all of them told us that the hospital Dr. and nurses are untouchable because of the back to work bill that is letting anyone working with covid patients can do anything they want to them. They are getting paid for these deaths and awarded for doing this to people.
We live in the United states of America, the land of the free ruled by the people not by the select few people who think they are God.
Sincerely Michaelle
Filter By Category

Age: 61
Location: MI
Became sick: 12/25/2021
First sought care: 12/27/2021
Admitted: 01/05/2022
To: South Bay hospital
Murdered: 01/16/2022
Cheryl Corsi

Age: 61
Location: CA
Became sick: 07/25/2021
First sought care: 08/01/2021
Admitted: 08/01/2021
To: Corona Regional and Kindred Rancho Cucamonga
Murdered: 08/17/2021
Edward H Hamlin III

Age: 50
Location: MI
Became sick: 09/23/2021
First sought care: 09/25/2021
Admitted: 09/25/2021
To: Mercy Health
Murdered: 10/10/2021
Nick Percy

Age: 68
Location: CA
Became sick: 07/22/2021
First sought care: 07/23/2021
Admitted: 07/23/2021
To: Sharp Memorial Hospital
Murdered: 08/08/2021
David Charles Coleman

Age: 61
Location: MI
Became sick: 11/27/2021
First sought care: 12/05/2021
Admitted: 12/05/2021
To: Munson Hospital
Murdered: 12/19/2021
Edward Smith

Age: 64
Location: MN
First sought care: 07/26/2021
Admitted: 07/26/2021
To: Woodwinds, U of MN, Bethesda LTAC in St Joe's bldg
Estelle Senopole

Age: 58
Location: MT
Became sick: 10/09/2021
First sought care: 10/09/2021
Admitted: 10/09/2021
To: Billings Clinic Hospital
Leslie (Les) John Knutson

Age: 67
Location: SC
Became sick: 08/10/2021
First sought care: 08/20/2021
Admitted: 08/20/2021
To: Conway Medical Center
Murdered: 09/12/2021
Georgette Guccione

Age: 60
Location: MI
Became sick: 11/13/2021
First sought care: 11/17/2021
Admitted: 11/17/2021
To: Sparrow Hospital Ionia Michigan
Murdered: 12/13/2021
Jeffrey Jay Marshall

Age: 63
Location: IL
Became sick: 03/14/2021
First sought care: 03/27/2021
Admitted: 03/28/2021
To: Delnor Hospital
Murdered: 05/15/2021
James A Evans

Age: 69
Location: IL
Became sick: 10/15/2021
First sought care: 10/15/2021
Admitted: 10/15/2021
To: AMITA Adventist La Grange Memorial Hospital
Murdered: 10/25/2021
Eugeniusz Lichosyt
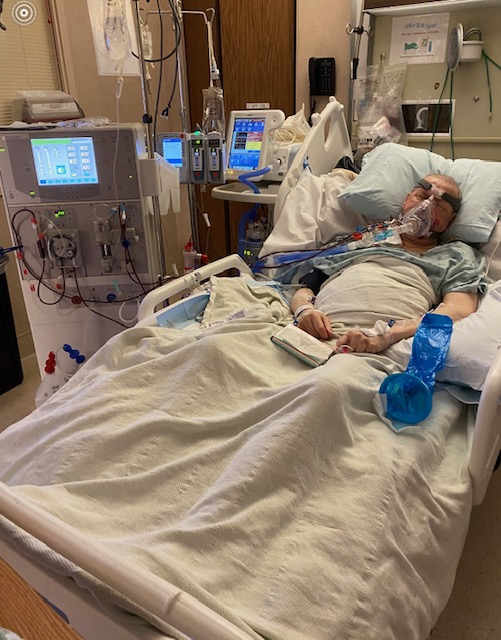
Age: 71
Location: OR
Became sick: 05/03/2021
First sought care: 05/20/2021
Admitted: 10/25/2023
To: My Hood, Legacy Emanuel and Portland Adventist.
Howard “Joe” Savage

Age: 77
Location: VA
Became sick: 10/05/2021
First sought care: 10/07/2021
Admitted: 10/13/2021
To: Reston Hospital
Murdered: 11/02/2021
Spencer James Rainey

Age: 54
Location: CA
Became sick: 08/01/2021
First sought care: 08/13/2021
Admitted: 08/13/2021
To: Kaiser Permanente, Santa Clara, CA
Lena Spasioti

Age: 50
Location: ID
Became sick: 08/24/2021
First sought care: 09/05/2021
Admitted: 09/05/2021
To: St. Alphonsus
Laura L. Baker

Age: 69
Location: TX
Became sick: 11/29/2021
First sought care: 12/12/2021
Admitted: 12/14/2021
To: The Hospitals of Providence, El Paso, TX
Murdered: 01/23/2022
Joseph Ayoub

Location: IL
Became sick: 12/21/2021
First sought care: 12/22/2021
Admitted: 12/22/2021
To: Local Medical Center
Murdered: 12/29/2021
Mary Lou Fosnaugh
Age: 54
Location: MI
Became sick: 09/12/2021
First sought care: 09/14/2021
Admitted: 09/14/2021
To: Henryford
Murdered: 09/29/2021
Michael Norman

Age: 61
Location: CA
Became sick: 09/02/2021
First sought care: 09/12/2021
Admitted: 09/12/2021
To: Shasta Regional Medical Center
Murdered: 10/26/2021
Vickie Michelle Houser

Age: 72
Location: WA
Became sick: 12/23/2021
First sought care: 01/02/2022
Admitted: 01/03/2022
To: St Vincent’s Portland OR
Cyndee Ellis

Age: 74
Location: FL
Became sick: 08/19/2021
First sought care: 08/10/2021
Admitted: 08/10/2021
To: UF Health Shands Hospital
Murdered: 08/28/2021
Morris “Tony” Hollingsworth

Age: 54
Location: PA
Became sick: 11/09/2021
First sought care: 11/09/2021
Admitted: 11/14/2021
To: Evangelical Community Hospital Lewisburg Pa
Murdered: 11/18/2021
Matthew Smith
Age: 43
Location: MN
Became sick: 08/07/2022
First sought care: 08/10/2022
Admitted: 08/10/2022
To: First to Essentia Health in Virginia Minnesota. Then taken by ambulance to St. Mary's Hospital in Duluth Minnesota
Murdered: 08/29/2022
Allison (Lakoskey) Thompson

Age: 73
Location: WA
Became sick: 08/03/2021
First sought care: 08/10/2021
Admitted: 08/10/2021
To: St Peters
Murdered: 09/01/2021
Dan Swecker
These are just a few of the cases archived by our COVID-19 Humanity Betrayal Memory Project, and there are more being reported by survivors and families of victims every day. If you would like to help with this project, please consider becoming part of the Task Citizens Force Against Instutional Capture And Crimes Against Humanity, a FormerFedsGroup Freedom Foundation mission.