
Feel betrayed
Age: 64
Location: NJ
Became sick: 08/13/2021
First sought care: 08/21/2021
Admitted: 08/21/2021
To: Virtua Hospital, Marlton , NJ
Murdered: 09/08/2021
Richard Eaton



Michael became ill with covid symptoms on 8/6/21 two days after I became ill. The two days following we spoke to a doctor here in Florida who, after a telehealth visit, prescribed us the Ivermectin/Hydroxychloroquine regime. Unfortunately, all pharmacies in our area were low with both medications and we’d have to wait for these meds for quite a few days. Four days after Michael became ill on 8/10/21, He complained about his chest feeling heavy. I suggested that we both go to local standalone ER, and we chose AdventHealth.
When we first arrived, I had my husband sit while I went to the front desk. We were both masked with the N95 masks, and I immediately told reception that we both were covid positive. I told the woman working reception that my husband had a heavy feeling in his chest, and I was looking to be checked as well. She asked if we were vaccinated, and I told her we were not. She was very rude and so much so I asked her if we should leave and go elsewhere. A few minutes later while I was finishing up paperwork, Triage called my husband back and shortly after, they called me back.
When I arrived in Triage, they had taken all my husband’s vitals and given him an EKG. They told me his oxygen was at 93 stating that was low and that they were concerned. They took us to our rooms and immediately separated us from each other. I heard the doctor first examine my husband. I could hear them talking but not so much what they were actually saying. The doctor then came over to my room and he asked if I and my husband were vaccinated. I am sure he had already asked my husband but asked me again. I told him we were not, and he pointed his finger in my face, got really close and told me we should be ashamed of ourselves.
He then told me that it looks like, based on my vitals, that I was the lucky one and my husband was not. Told me he wanted to admit my husband as his x-rays did not look good and that his could be life or death. My husband was admitted, and I was given 5 minutes to say good-bye before they escorted me out of the ER. I asked them if I could stay with him until he at least got a room at the hospital itself, and they told me no and I had to leave. I also told them I had just received a call earlier that morning that our prescriptions for Ivermectin and Hydroxychloroquine were ready for pick-up. And could I bring them back and have them administer that medication to Michael.
The nurse told me that was not their protocol, was not proven to help with covid and would not be allowed. That was the last time I saw my husband alive. Hours later, Michael finally got a room at AdventHealth Hospital in Altamonte Springs, Florida. Michael was put on a biPAP and sent to ICU for evaluation. I had not received any communication regarding his medications, regimens or any action plans from the doctors or nurses. Occasionally, I received a call from a nurse at night that would tell me how he was doing but the conversations were vague.
During this time, Michael’s parents had been speaking to one of the doctors who was helping him and after hours of pleading, he agreed to give my husband Ivermectin. It was a low dose, and it was prescribed for 5 days. During this time, just after 24 hours, Michael was improving. On 8/20/21, before he was to take his 4th round of Ivermectin that was given to him by the nursing staff, he dropped the pill while trying to take it and because there was no hospital staff in the room with him, he tried to reach it himself and according to staff, he had an episode. We aren’t really sure what exactly happened.
All hospital and doctors’ notes skip over this “episode” and nothing is mentioned about this. They did state falsely he had all 5 doses of the Ivermectin when he only had 3 doses. When this “episode” occurred, a nurse had called me to tell me of it. She stated he dropped the pill and panicked when he went to pick it up and his oxygen dropped so they sedated him. This is one of the very few updates I had ever received from this hospital staff. They told me they would call me later and let me know how he was doing.
Later that evening, I received a text from my husband. He told me he had made a mistake and dropped the pill and “the first thing they wanted to do was shove a hose down my throat”. Then he stated he argued and asked for just the oxygen mask and they sedated him to keep him calm. He said he felt like he was in a cloud. After that, he stopped texting, and it was the last time I ever heard from my husband again. About an hour later, the nurse called me to tell me he was doing better, and they were moving him to another floor where less severe cases of covid stay. She explained to me he stopped texting because he was highly sedated, and he was just falling in and out of sleep.
The next morning at about 9:45, a doctor called me to inform me that my husband was placed on a ventilator. She was cold and unsympathetic. Then she told me that his oxygen dropped, and she told him if she didn’t ventilate him, he would die. He was ventilated without anyone’s knowledge or consent, and we feel he wasn’t in any position to provide consent himself as he was highly medicated. What we read in the hospital notes is that he was delirious and in sever distress.
So although he had a do not intubate order, she said he rescinded it. And because his status was unclear, she intubated him. We never received any contact beforehand that his condition was deteriorating, or he was not doing well. Again, the last we heard that night before was that he was improving. Please see the notes below (copied from the actual medical records).
08/13/2021 – No events overnight, vitals reviewed, labs reviewed.
BiPAP FiO2 100% overnight, switched to HHFNC this morning 50 lt/min; 100%.
7.41 / pCO 38 / pO 65 on BiPAP 100%
Proning.
08/14/2021 – No events overnight, vitals reviewed, labs reviewed.
On HFNC
Increased D-dimer to 7.7
Proning.
08/15/2021 – Patient spent night on BiPAP on FiO2 100%, tolerated well. Proning during night.
Evaluated at bedside, no acute distress, speaking full sentences. On BiPAP 100% today.
Family and patient have been requesting to get Ivermectin. They are aware of FDA, NIH and IDSA
recommendations regarding Ivermectin. It was clearly explained about the lack of convincing evidence of its
benefit at this time. There is insufficient evidence for the COVID-19 treatment with Ivermectin. They insisted and
stated that assume full responsibility about any side effect. They verbalized understanding about the potential
side effects I listed them. Additional, sufficiently designed clinical trials are needed to inform decisions.
8//16/21. The patient is breathing fairly well. No chest pain or palpitations. and no nausea vomits or diarrhea. No
bleeding. Still requiring BiPAP q.h.s.. He is now off the BiPAP and he is on 50 L 100% FiO2 high flow heated
humidified nasal cannula
08/17/2021. The patient has been using BiPAP at night 100% FiO2 and then during the day trials of high flow
heated humidified nasal cannula.
Chest x-ray from yesterday with bilateral infiltrates slightly improved when compared to previous films.
8/18/21 The patient is breathing better today. Currently on high flow heated humidified nasal cannula. 60 L 100%
FiO2. Slept with BiPAP. Denies any chest pain palpitations nausea vomits or diarrhea. No bleeding.
08/19 – No events overnight, vitals reviewed, labs reviewed.
Was on HHFNC during the day, today had an episode of desaturation and tachypnea, had to be placed on BiPAP.
08/21 patient was desaturating into the 60s, delirious, severe distress, I was told by the nurse and the respiratory
therapist that he was a do not intubate however he did say he recent today and wanted to be intubated, at this
point since his status was unclear and he was in severe distress I went ahead and intubated the patient
Once Michael was placed on the ventilator, Michael’s parents and I tried speaking to doctors and staff about trying high dose vitamin C therapy. One of the doctors told us that vitamin C therapy would not help. We asked if we could try regardless. He went on to tell us how vitamin C could harm his kidneys and then eventually said if he were to agree to administer high dose vitamin C, we’d have to sign a DNR. He gave us an ultimatum and we found this very disturbing. Of course, we never agreed to that. We were contacted by palliative care and that representative was very unsympathetic as well. She actually cracked some jokes and tried to be funny while speaking to us.
I believe she also asked about a DNR. We were pressured quite a bit from hospital staff during the time my husband was ventilated about an DNR. I’m sure they pressured him as well. We did speak to nurses every evening for status updates, but we had to make the call. If we didn’t, we would get any updates and the updates were just about his oxygen and blood gases. We only seemed to speak to doctors if we requested it. We had a doctor tells us at one point they were watching his kidneys but in his medical records it states he had acute kidney injury.
It was never disclosed to us the numerous medication they were administering to him or the damage they could cause, starting with remdesivir that was given to him before he was even transported from the ER to the hospital. Our consent was never asked for anything they did to him or gave him during times when he couldn’t make a sound decision for himself or during the days he was ventilated.
The called my cell phone the early morning of 8/31/21 to tell me Michael was dying. The nurse I spoke to was abrupt, mean and rude with my husband’s parents and myself. She asked us to agree to the DNR and we started by saying no but she became almost angry. And told us he was dying and that if we didn’t agree to the DNR, they’d be cracking his chest open, and he’d be going through a lot of traumas. We then agreed to the DNR. After 3 weeks and obviously too late, they let us go to see him before he died. We walked through the covid ICU floor. It was heart wrenching and disturbing to see how many people were waiting to die, all on ventilators. There had to have been at least 30 people that we passed before we got to my husband.
We were not allowed to go in to see him until we were fully gear in HAZMAT suits, gloves, masks, shields on top of the masks. I was unable to touch my husband with my bare hands. They nurse came in right as we got there and put something in his IV and he started to slip away. It haunts me today because I do believe whatever the nurse gave him expedited his dying. Fifteen minutes after the IV was given, he was gone. A doctor came in after he passed to verify, he was gone and to speak to us. He too was very undetached with no sympathy, cold, just like the nurse who called us hours before.
This doctor told us how all those people we saw and passed were dying and how the man next to my husband was in his 30’s. My husband’s mother told him the hospital protocols obviously aren’t working and he said nothing and left the room. As you can see, my husband was given numerous medications all without our knowledge or consent. We were never kept informed as to his progress and deteriorating condition from the doctor’s and the nurses were very vague. In addition, the doctor’s progress notes have multiple errors. We have been reaching out to different attorney’s looking for help with this and it seems no one wants to get involved.
Filter By Category

Age: 64
Location: NJ
Became sick: 08/13/2021
First sought care: 08/21/2021
Admitted: 08/21/2021
To: Virtua Hospital, Marlton , NJ
Murdered: 09/08/2021
Richard Eaton
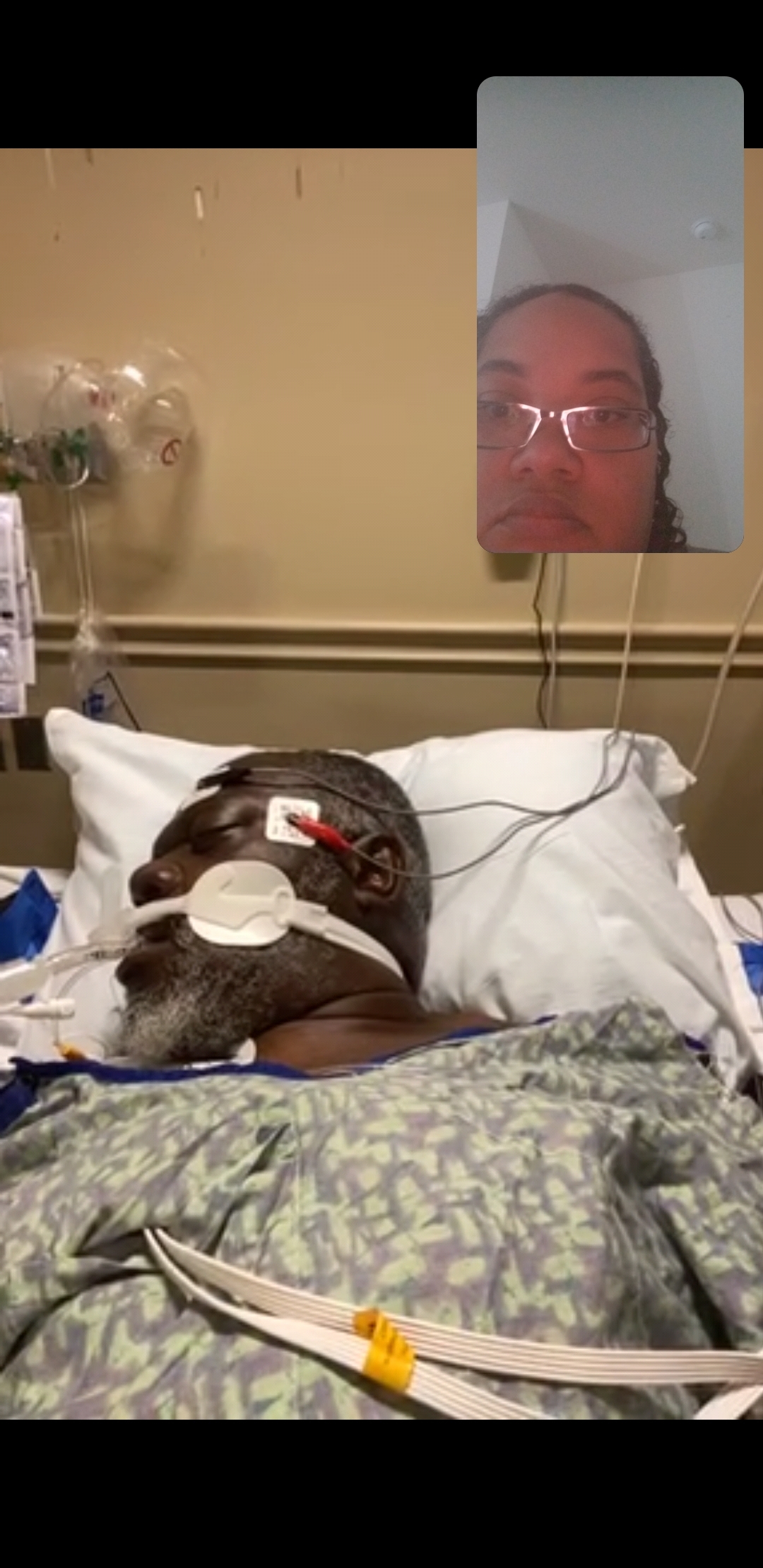
Age: 63
Location: AL
Became sick: 11/12/2021
First sought care: 11/15/2021
Admitted: 11/15/2021
To: Baptist East , 400 Taylor Rd
Murdered: 12/13/2021
William Peagler Jr.

Age: 74
Location: PA
Became sick: 12/29/2021
First sought care: 12/31/2021
Admitted: 01/07/2022
To: UPMC Altoona
Murdered: 01/12/2022
Ruthford Fredrick Penrod

Age: 73
Location: OH
Became sick: 12/23/2021
First sought care: 12/26/2021
Admitted: 12/29/2021
To: Clinton Memorial Hospital
Murdered: 01/17/2022
Connie Mae Moore

Age: 73
Location: AZ
Became sick: 11/20/2021
First sought care: 11/23/2021
Admitted: 12/01/2021
To: Havasu Regional Hospital
Murdered: 12/15/2021
Raymond Delworth

Age: 61
Location: FL
Became sick: 06/25/2021
First sought care: 07/04/2021
Admitted: 07/04/2021
To: Mease Countryside Hospital Safety Harbor, Florida
Murdered: 08/11/2021
Jeffrey R Smith

Age: 61
Location: FL
Became sick: 07/16/2021
First sought care: 07/20/2021
Admitted: 07/22/2021
To: Port Orange, Florida Halifax
Ginae Lee Karoub

Age: 54
Location: GA
Became sick: 11/03/2021
First sought care: 11/07/2021
Admitted: 11/14/2021
To: Unknown
Adam Farber

Age: 43
Location: CA
Became sick: 03/29/2021
First sought care: 04/13/2021
Admitted: 04/20/2021
To: I went to the hospital after 2 or 3 weeks. When I started having more paresthesia in my legs
S.H. (anonymous)

Age: 84
Location: CA
Became sick: 09/16/2022
First sought care: 09/18/2022
Admitted: 09/18/2022
To: Kaiser Permanente – 2295 S. Vineyard Ave., Ontario, CA
Murdered: 09/30/2022
Kenneth Slaughter

Age: 68
Location: WI
Became sick: 01/01/2022
First sought care: 01/10/2022
Admitted: 01/10/2022
To: Waukesha Memorial/ProHealth Care
Murdered: 01/21/2022
Michael O’Dell

Age: 34
Location: AZ
Became sick: 11/11/2021
First sought care: 11/17/2022
Admitted: 11/17/2021
To: St. Joseph's Carondalet Hospital
Murdered: 12/11/2021
Evangeline “Vangie" Young

Age: 67
Location: NV
Became sick: 07/20/2021
First sought care: 07/27/2021
Admitted: 08/08/2021
To: Centennial Hills Hospital, Las Vegas, NV
Murdered: 08/19/2021
Charles Anthony Malito

Age: 48
Location: OH
Became sick: 11/11/2021
First sought care: 11/17/2021
Admitted: 11/17/2021
To: Avita Hospital Ontario, Oh and Cleveland Clinic Main Campus, Cleveland, Ohio
Murdered: 05/27/2022
Jeffrey Simon Perelka

Age: 40
Location: MI
Became sick: 12/02/2021
First sought care: 12/13/2021
Admitted: 12/13/2021
To: Three Rivers Hospital and Ascension Borgess Hospital
Murdered: 01/05/2022
Michael Hall

Age: 69
Location: GA
Became sick: 08/18/2021
First sought care: 08/19/2021
Admitted: 08/22/2021
To: St. Mary’s Hospital
Murdered: 09/06/2021
Larry W. Roberts

Age: 44
Location: AZ
Became sick: 11/11/2021
First sought care: 11/20/2021
Admitted: 11/21/2021
To: St Joseph
Alegra Acosta-Young

Age: 48
Location: IA
Became sick: 12/19/2021
First sought care: 12/20/2021
Admitted: 12/28/2021
To: Mercy Westlake
Murdered: 02/28/2022
Darryl Van Holton

Age: 19
Location: TX
Became sick: 08/10/2021
First sought care: 08/18/2022
Admitted: 08/21/2021
To: North East Methodist San Antonio
Murdered: 08/25/2021
Justin Crocker

Age: 79
Location: KS
Became sick: 09/22/2020
First sought care: 10/06/2020
John H Engelcke

Age: 80
Location: GA
Became sick: 12/24/2021
First sought care: 12/28/2021
Admitted: 12/30/2021
To: St Mary's Athens GA
Murdered: 01/11/2022
Gary Phillips
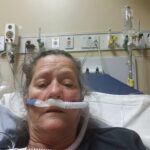
Age: 64
Location: NV
Became sick: 10/08/2021
First sought care: 10/15/2021
Admitted: 10/15/2021
To: Mountain View Hospital and Pam Rehab
Regina Bell

Age: 69
Location: VA
Became sick: 10/01/2021
First sought care: 10/04/2021
Admitted: 10/06/2021
To: Santara Martha Jefferson
Murdered: 10/20/2021
Sherman Herritt

Age: 67
Location: CA
Became sick: 02/20/2022
First sought care: 02/27/2022
Admitted: 02/27/2022
To: Kaiser
Murdered: 06/14/2022
Connie Vu
These are just a few of the cases archived by our COVID-19 Humanity Betrayal Memory Project, and there are more being reported by survivors and families of victims every day. If you would like to help with this project, please consider becoming part of the Task Citizens Force Against Instutional Capture And Crimes Against Humanity, a FormerFedsGroup Freedom Foundation mission.